Trigeminal neuralgia (also known as tic douloureux) is a chronic pain condition affecting the fifth cranial nerve (1). There are twelve cranial nerves that emerge from the brain and cranial nerve V carries sensation from the face to the brain. Trigeminal neuralgia occurs at a rate of 4.3 per 100,000 people per year (2). There are two main types: classic trigeminal neuralgia and atypical trigeminal neuralgia (3). It is vital to consult with a specialist and confirm the diagnosis, which may include neurological testing and MRI of the brain (4). Both of these diagnoses can be extremely painful, debilitating, and especially frustrating when multiple traditional treatment options are not effective in relieving pain.
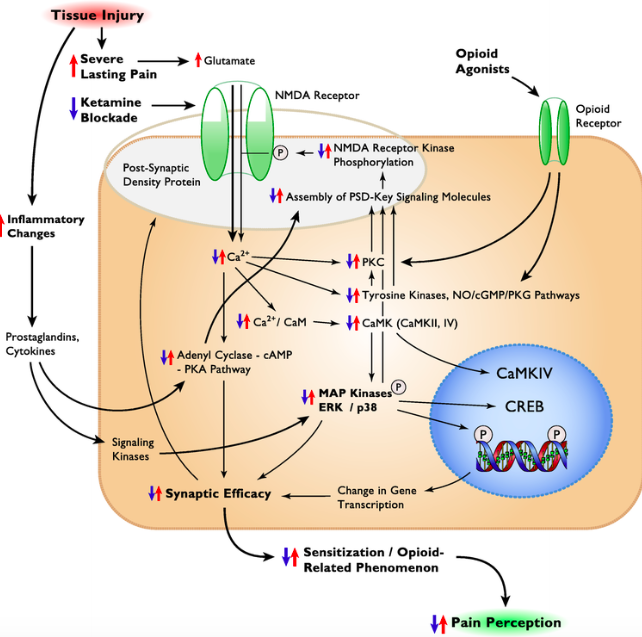
Recent studies are showing that ketamine used “off-label” may be effective in the treatment of various mood and pain disorders. Ketamine works on the N-Methyl-D-aspartate (NMDA) receptor, which is stimulated by glutamate neurotransmitter. Blocking this NMDA receptor may play a role in relieving acute and chronic pain syndromes. In neuropathic pain, ketamine seems to reset the hyper-sensitized pain receptors within the central nervous system (5).
In sensitization and opioid tolerance-related phenomena, pathologic pain is an expression of neuronal plasticity (6).
Ketamine has been FDA approved for 50+ years and is now a generic drug. It is challenging to get funding on generic drug research. Unfortunately, large-scale placebo controlled trials are scarce in the treatment of trigeminal neuralgia (2). Given this limitation, we will review some of the recent research and case reports available.
In an article published in 2017, researchers took 100 adult patients with trigeminal neuralgia and randomized them to receive either ketamine (50 patients) or lidocaine (50 patients) infusions (7). The ketamine infusions were 0.4mg/kg and given over 30-35 minutes and lidocaine infusions were 5mg/kg and given over 30-35 minutes. This was performed consecutively every 4th day for 3 infusions. They found that ketamine had significantly longer duration of pain relief at 2 weeks, 1 month, 2 months, and 3 months without serious side effects for up to three months. The ketamine infusion group also had a decrease in the use of carbamazepine by patients.
A case report from Johns Hopkins University School of Medicine was presented during the 2018 World Congress on Regional Anesthesia & Pain Medicine (8). Dr. Torrie et al. reported a 40 year old male with chronic, refractory left-sided atypical trigeminal neuralgia. The patient received one infusion of ketamine (20mg bolus and then 0.5mg/kg/hr for four hours). He reported 100% pain relief at 7-day follow-up, then 50% reduction at his one and four-month follow-up appointments. Furthermore, he was able to stop all of his pain medications after the infusion.
As you can see from the research above, there are variations in dosing, timing, and sequence of infusions. This makes sense because ketamine is being used off-label and there are no current FDA guidelines on protocol. Accordingly, you will find that different physicians are using ketamine with different protocols. Please note that these studies and case reports have a small sample size, so your results will vary!
Regardless of which doctor you choose, it is important to have a well-qualified physician with a background in ketamine use. Also, it will be prudent to have continuous cardiac rhythm, oxygen level, respiratory rate, & blood pressure monitoring during infusions for chronic pain.
If you have any questions, please contact us or get a free consultation today!
References:
1. “Trigeminal Neuralgia.” Mayo Clinic, Mayo Foundation for Medical Education and Research, 26 July 2017. www.mayoclinic.org/diseases-conditions/trigeminal-neuralgia/symptoms-causes/syc-20353344.
3. “Trigeminal Neuralgia.” Wikipedia, Wikimedia Foundation, 30 Sept. 2018, en.wikipedia.org/wiki/Trigeminal_neuralgia.
4. Krafft, Rudolph M. “Trigeminal Neuralgia.” AAFP Home, 1 May 2008, www.aafp.org/afp/2008/0501/p1291.html.
5. Boyle, Annette. “Ketamine Resets System for Normal Pain Processing in Complex Syndrome Patients.” U.S. Medicine, 5 Aug. 2017. www.usmedicine.com/agencies/department-of-defense-dod/ketamine-resets-system-for-normal-pain-processing-in-complex-syndrome-patients/.










Stop racing to the next destination. Discover Alan Watts' wisdom on viewing life as a dance, not a marathon - and why this perspective shift can help you enjoy the process of being alive.